Bite me. You might as well go outside and shout it loud, because there isn’t enough DEET in your medicine chest to fend off Culex pipiens, Anopheles, Aedes vexans, and dozens of other species of infected mosquitoes blanketing the United States. Right this minute. West Nile virus season is in full swing—consider August 2012 a preview.
Don’t get me wrong.
Health organizations, federal, state and local, have spent buckets of money on nice-looking, easy-to-understand websites that calmly advise citizens to douse ourselves with bug spray, wear light, long-sleeved clothing (think Out of Africa), eliminate standing pools of water, and, of course, just stay inside the damn house until the Center for Disease Control sounds the all-clear.
All good. But hardly sufficient.
West Nile virus—how it got here, how it travels, how it kills, and how health officials could, but fail to mount the most effective responses—is a complicated story, a cautionary tale, some say, about power, ego, bureaucracy, preparedness, ignorance, incompetence, and disparate champions whose voices routinely go unheard and whose counsel is largely ignored.
 Right now, the highbeams are on Dallas, Texas, “Ground Zero” for West Nile—and Mayor Mike Rawlings has indeed declared a state of emergency in the municipality. As the number of victims escalates, however, so does the anxiety of state and local officials, as well as the complaints of constituents, who’ve begun to question and criticize the city’s response to the health crisis.
Right now, the highbeams are on Dallas, Texas, “Ground Zero” for West Nile—and Mayor Mike Rawlings has indeed declared a state of emergency in the municipality. As the number of victims escalates, however, so does the anxiety of state and local officials, as well as the complaints of constituents, who’ve begun to question and criticize the city’s response to the health crisis.
They have a point
An epidemiologist who has spent his life researching vector-borne diseases, and one of the first to face-down the West Nile virus in 1999, says Dallas, the ninth-largest city in the U.S., is facing an escalating threat: given the sizeable population (1,223,229), the number of victims who’ve already contracted the virus, the number of fatalities reported at the end of August, and the fact that September and October are likely to represent a zenith for the disease, the prospect isn’t good.
In fact, estimates this health expert, 98 to 99 percent of the population of Dallas is probably still susceptible to the virus, which means—“If you don’t stop the proliferation of mosquitoes right now and impose real mosquito control across Dallas County”–disaster.
When West Nile virus was first diagnosed in New York, 1999, the race was on to identify which strain of mosquito was carrying the disease. The first and most likely vector was Culex pipiens, an urban species of mosquito found in drainpipes, sewers, and other city receptacles—and active only during the day.
Now, here’s the problem, and the key to understanding what real mosquito control entails: To eliminate infected mosquitoes via the spraying of chemical pesticides, you need to know exactly which species you are dealing with; you need to know exactly when that particular species is active; you need to know where it resides, and you need to know exactly which kind of pesticide to use as well as the right concentration.
What, where, when, which, and how much.
An analogy from a virus-hunter who’s been there and done that: You step on a rusty nail, and rush to the doctor for treatment. He doesn’t give you a random vaccine, doesn’t sit back and say, “Hmmm . . . how about a flu shot, guy? That might help.” No, your GP gives you a tetanus shot, a specific remedy applied within a specific time period to combat a specific infection.
That’s not always what’s happening as health officials in Texas and other places struggle to eliminate the threat.
Not by a long shot.
In too many cases, officials are applying generic pesticides at non-specific times of day to random sites, flying, one might say, by the seat of their pants.
In New York, for example, weeks after they’d targeted c. pipiens, researchers discovered that two additional species of mosquitoes, one of which was active during the night, were also transmitting West Nile virus to human targets in New York.
Up to that point, officials there had only been spraying during the day, but luck was both with and against officials in New York: their timing was off, but they did discover that the toxicity of the spray used to eliminate the first species of mosquitoes, c. pipiens, was equally toxic for the other two. You might want to think about that . . .
Wait.
It gets worse
In 2012, epidemiologists have identified as many as 40 different species of mosquitoes operating in specific regions and states across America—species active at different times of day and night, species with different feeding schedules, species which inhabit different environments (c. pipiens is a ‘canopy feeder’ so ground spraying is useless), species with disparate longevity and particular population densities. And these mosquitoes like to travel.
Right now, Mississippi, Louisiana, Oklahoma, South Dakota, and California are running close seconds to Texas in terms of the threat from West Nile virus, but in each of these states, and in separate pockets within each state, the challenge confronting officials intent on eliminating particular species of mosquitoes attacking particular geographic areas is enormously complex.
More than a decade after the disease made its initial appearance in New York (an Army researcher at Ft. Detrick speculates its mosquito-host might have been a stowaway on a flight from Israel) the CDC, state and local health officials across the country continue to throw stones at the rising threat of epidemic via disparate and uncoordinated responses dictated by local budgets, small-town politics, and widespread ignorance about the nature and seriousness of zoonotic disease.
Here’s how it works: Zoonotic diseases recruit carriers from “garbage wildlife”–rodents, birds, rabbits, raccoons, possums, fleas, lice, monkeys, ticks, dogs, cats and bats—all locked and loaded with lethal doses of infectious agents.
In addition to West Nile virus, a partial list of zoonoses—viruses capable of skipping across species from animals to humans—includes Dengue fever, Cholera, Smallpox, Anthrax, Tularemia, Ebola, Q-fever, HIV-1, HIV-2, Hantavirus (aka Hemorrhagic fever), and of course, the Spanish flu which, between 1918 and 1919, killed a third (some say half) of the global population.
Take a minute
H1N5. A new (2011), man-made virus conjured into an already too-extensive collection of bug-bites-man killers, and, according to Dr. Paul Keim, Chair of the US National Science Advisory Board for Biosecurity (NSAAB), “the most potentially dangerous pathogen in existence.” 
Now, you’d think the U.S. government would be all over this.
Last December, the New York Times Editorial Board took issue, briefly, with the decision of researchers to publish a “how-to” guide to building a deadly, air-borne virus capable of mammal-to-mammal transmission (biowarfare concerns, can you believe it?), but scientists want their ten minutes of fame as much as anyone else. Note to Yoshihiro Kawaoka, head of the team that blew breath into H1H5: “I am become death”–J. Robert Oppenheimer.
But back to the point: Zoonotic diseases, whether they materialize on their own or jump into the human population courtesy of Doctor Strangelove, pretty much enjoy an open field.
Free-range plague, so to speak.
There is nobody, no health agency in the United States, that has any kind of specific, designated investment or interest in wildlife surveillance.
When vector-borne disease erupts, America is invariably taken by surprise.
Russia scores–U.S. misses
This isn’t how it works in places like Russia, by the way, where $750 million a year is committed, via the Defense Threat Reduction Agency (DTRA), to zoonotic research, integrating animal and human research in the hope their scientists can find and obliterate infected wildlife, tainted vectors, before virulent mosquitoes, rabid coyotes, or plague bearing rodents begin attacking human victims.
 Russia understands the consequences of biological disaster: at the turn of the last century, the country reeled under the onslaught of Plague. The government responded by creating the Russian Anti-Plague System, a species-neutral approach to zoonotic threat. The strategy turned on the active surveillance of possible vectors, location of rodent sites, and the construction of incredibly detailed maps targeting shifting hotspots. From an epidemiological standpoint, it stands as an extraordinary achievement.
Russia understands the consequences of biological disaster: at the turn of the last century, the country reeled under the onslaught of Plague. The government responded by creating the Russian Anti-Plague System, a species-neutral approach to zoonotic threat. The strategy turned on the active surveillance of possible vectors, location of rodent sites, and the construction of incredibly detailed maps targeting shifting hotspots. From an epidemiological standpoint, it stands as an extraordinary achievement.
Here, in the U.S., it’s the other way around. Once human targets start falling, the CDC starts to work its way backward as it did in the case of West Nile virus. Human infections increase, human fatalities start piling up, and the CDC launches an investigation into possible causes, collaborating only occasionally with the veterinary community or any entity outside the huge public health system it leads. Many officials at state and local levels are former CDC employees or contractors.
Congress sends a lot of money to the CDC (its budget request for 2013 is $13 billion+), but those funds don’t always come without strings. One researcher says too much goes toward the latest ‘disease de jour,’ and it is true that the CDC has used taxpayer monies to delve into hot-button issues like AIDS, abortion and contraception. In 1995, the CDC even conducted a study of firearm injuries that concluded guns were a public health threat. Okay, the gun study is long-gone, but you get the point.
No one is saying the CDC isn’t a standup organization when it comes to national emergencies—TB, E.coli, SARS, and the like. But the Director is appointed by the President; overseas assignments are vetted by senior political appointees in the administration, and the organization’s research, predictably, often moves parallel to the prevailing political winds.
The USDA, on the other hand, exists to protect valuable agriculture and commercial livestock. It focuses on animals, not the kind you find rooting around in your garbage when you turn on the porch light and you know enough not to pet, but on the multi-billion supply of livestock the U.S. depends on for export as well as domestic sale and consumption. We’re talking about plants and animals that deliver cash returns.
Leaders of big federal agencies report to the White House, reporting to Congress, generally, only when they get it wrong and need to save their own skins or go after someone else’s. Cynical, perhaps, but let’s just cop to it and move on. Congress was only mildly interested in the problems that attended the advent of West Nile virus into the United States in 1999, and because the disease has crept along quietly, at least until the summer of 2012, legislators have allowed the issue to slip off their screens.
Mistake.
When West Nile virus first made its appearance in the U.S. 13 years ago, efforts to identify the unknown disease killing seniors in several New York boroughs were delayed and complicated by the worst practices of federal, state and local bureaucracies—turf wars, misguided regulations, organizational stovepipes, a lack of cooperation and communication, poor or misdirected funding, rivalries between scientific disciplines, and the willingness of CDC officials to compromise the timeliness of the investigation, rather than admit their organization lacked the diagnostic resources and expertise to handle a crisis of this kind alone.
 As dismal as this assessment may be, some predict there may be more sinister consequences down the road: How can we expect a national health system such as the one we have, a system struggling erratically to eliminate a mosquito-borne illness, to deal with more urgent biological cataclysms, either natural or man-made?
As dismal as this assessment may be, some predict there may be more sinister consequences down the road: How can we expect a national health system such as the one we have, a system struggling erratically to eliminate a mosquito-borne illness, to deal with more urgent biological cataclysms, either natural or man-made?
Critics say America’s complacency in regard to West Nile virus, the concerns of citizens about how spraying might affect their koi ponds or organic gardens—as opposed to the attention we might expect a disease with a 10 percent fatality rate to generate—signals a failure by health officials, the government, and the media to tell the right story about zoonotic disease in general, and West Nile virus in particular.
Let’s do it.
Buggered
According to Richard Knox, National Public Radio science correspondent, there are more than 100,000 Americans (some sources report as high as 500,000) who have contracted West Nile virus over the last decade, many without knowing it. These survivors, “dead end hosts,” now carry the viral aftermath (as well as immunity to another bout) within their bodies.
Let’s call them the lucky ones.

viruses that cause West Nile
Encephalitis, the medical definition for West Nile virus, is a killer, and there is no ‘cure,’ just varying levels of response (mild, moderate, and fatal) to the disease.
Scientists have tested antibodies on mice, but it’s still a no-go for people. The odds the virus will tunnel into the brain (the worst outcome) are significant for the 40 percent hit hard by the disease (encephalitis), with prospects especially bad for people over 50, the very young, and individuals with weakened immune systems. Pathologist who’ve performed necropsies on infected birds have also questioned the notion that West Nile encephalitis can really bypass the brain—‘non-neural involvement—since avian samples taken from birds thought to be only mildly infected have also shown traces of neurological invasion. More research needed here.
In Europe, where the West Nile virus appears cyclically, health authorities have had enough experience with the disease to know that the mortality rate is about 10 percent: Out of 500 people diagnosed with full-blown encephalitis, expect 50 fatalities. These are very serious numbers.
The virus enters the body through the bite of an infected tick or mosquito and lodges there, undiscovered, for ten to fifteen days. When the incubation period is over, the virus can attack the brain, triggering headaches, vomiting, fever, dehydration, convulsion, and coma.
The key, when the encephalitis virus strikes, is to identify the strain as quickly as possible.
STAT.
Without that speedy ID, treating the virus and combating its spread is impossible. Every hour of delay can mean an exponential increase in victims.
Scroll back—different strains of encephalitis are carried by different species, or populations, of mosquitoes, which infect victims, both human and animal, by feeding on them. And don’t forget: Each species of mosquito has different habits, different waking and sleeping times, and most importantly, different feeding times.
Pinpoint the right time of day, the right place, and the right group of mosquitoes, and spraying can eliminate the threat.
Spray the wrong group of mosquitoes, or the right mosquitoes at the wrong time of day—use the wrong pesticide, or dump the right chemicals in the wrong place—and the deadly transmission cycle continues unabated.
Easy to get it wrong
In September 1999, government health officials did exactly that, fumbling the ball for two long months before they were able to identify (not combat, not prevent, just identify) a strain of encephalitis killing birds and senior citizens in a borough of New York. After the fact, spokespersons and ‘experts’ determined to transform the debacle into ‘lessons learned’ strained to put a positive gloss on official mistakes and misdiagnoses.
Smallpox
“West Nile fever was a wake-up call for us,” said Dr. Alan Zelicoff, a physician at the Federal Center for National Security and Arms Control at Sandia National Laboratories in Albuquerque, N.M. “If the West Nile virus had been a more serious virus, like smallpox, it would have dispersed and spread across the country to hundred of thousands of people.”
Smallpox.
Hundreds of thousands of people.
Dr. Annie Fine, Director of the New York Health Department’s Division of Infectious Diseases and Bioterrorism, described New York’s response to West Nile virus in 1999 as analogous to the response the city might have mounted “…had the crisis been triggered by an act of bio-terrorism.”
In a clear attempt to tamp-down her language, (did she really say bioterrorism?), Fine quickly added that health officials in the U.S. should look forward, not backward to past mistakes.
Bottom line?
NYC-DOH and CDC had been given a valuable opportunity “to improve.”
Not reassuring.
The Scariest Story Never Told
The panic began in August 1999, in Queens and the Bronx, when an outbreak of an unknown strain of encephalitis killed several elderly residents and rapidly infected 38 others. Doctors, scientists, and health organizations raced to identify the virus, taking blood samples door-to-door in Queens and sending work crews out to blanket the city with pesticides they hoped would obliterate the mosquitoes that carried the disease.
New York health officials, working with the Center for Disease Control (CDC), encouraged New Yorkers to remain calm.

Dr. Tracey McNamara
What few people realized at that point was that encephalitis was also sweeping through the animal population in New York. When that fact did come to light, its import was not appreciated. And it was only later, after seven people in New York had died from the unfamiliar virus, that anyone would admit that with better cooperation, the race to identify the disease might have ended weeks earlier than it did, shortly after Dr. Tracey McNamara, Chief Pathologist at the Bronx Zoo, called officials at the CDC with her hunch that whatever was killing crows on the zoo grounds was also killing people.
The CDC wasn’t interested.
Indeed, on September 3, 1999, health officials in New York and at the Center for Disease Control publicly announced they had succeeded in identifying the strain of encephalitis sweeping across the boroughs of New York: It was the St. Louis virus (SLE), a deadly variant that causes seizures and paralysis.
The good news, according to CDC officials, was that the virus was not a new strain. It had attacked St. Louis (the epidemic that spawned its name) in 1933; hence, said officials, the medical community had a good deal of information about the virus and how to treat it.
Mistaken Identity
The CDC’s optimism seemed to quell public fears. In the Bronx, however, where encephalitis continued to claim human lives, the Chief Pathologist at the Bronx Zoo was not convinced. McNamara had noticed increasing numbers of crows dying in the area. When dead birds began to litter Zoo grounds, she decided to collect the corpses for necropsy and tissue analysis.
The identification posited by New York health officials and the CDC assumed that the mosquitoes carrying the St. Louis virus were contracting the disease from infected birds and then passing encephalitis to human victims.
But Dr. McNamara knew that birds should not have been affected by the St. Louis virus because, in this case, the birds represented what scientists call a reservoir population—animals which develop a natural resistance or ‘immunity’ to a disease to which they have already been exposed.
In other words, if the encephalitis in New York, as officials claimed, were the St. Louis virus, carried by c. pipiens, there would not be dead birds on the ground.
But there were.
The crows went first, followed by five Chilean flamingoes, a cormorant, a snowy owl, and an American bald eagle—and all at the Bronx Zoo.
It wasn’t long before Tracey McNamara was literally up to her elbows in tissue samples taken from the dead birds. This was a problem, because the longer the zoo’s pathologist worked with the samples, the more convinced she was that whatever killed the birds was a Level-3 biological hazard.
If you need to know exactly how dangerous that is, consider this: The Ebola virus represents a Level-4 hazard.

BL-4 Unit unavailable to McNamara’s team
Dr. McNamara and her staff had neither the safety equipment they needed—she was working in a Level-2 hood—nor did they have access to the antigens they needed to do the kind of sophisticated testing that could unequivocally identify the strain of encephalitis killing the crows and zoo birds.
CDC Drops the Ball, Claims the Credit
Tracey McNamara believed the CDC had both the equipment and diagnostic tools her team needed. On September 9, 1999—six days after the government health officials had offered the public the reassuring news that the outbreak constituted the reemergence of the familiar St. Louis virus, McNamara called the CDC again to ask for help and to voice her growing suspicion that there might be a link between the encephalitis killing seniors in New York and the encephalitis killing birds in the Bronx.
Once more, CDC officials brushed McNamara off. Researchers there, she was told, were overwhelmed with tissue taken from dead human beings, and they had neither time nor the inclination to test samples from the Bronx Zoo. Moreover, the mission of the CDC had nothing to do with wildlife research. Get lost.
Here it was—the unacknowledged caste system within the medical community that makes health agencies responsible for research into human diseases unwilling to work with veterinarians.
Despite the sudden outbreak of encephalitis in New York (transmitted by non-human carriers and host populations), important databases at the CDC remained off-limits to wildlife pathologists and the veterinary community throughout the investigation.
McNamara was still not deterred. She reminded researchers at the CDC that the St. Louis strain should not be killing the birds, or avian hosts that were part of the cycle, and that it was likely that the strain of encephalitis devastating the avian population remained unidentified.
The CDC, sticking with their public pronouncement that St. Louis virus was to blame for human fatalities in New York, told McNamara it was had to be another, separate virus, Eastern Equine encephalitis, for example—killing crows and horses.
Were officials at the CDC right? Was it just coincidence that human and animal populations were dying simultaneously from different strains of encephalitis in the same, small geographic area?
The Games Begin
McNamara’s reason and her experience with wildlife disease detection told her it wasn’t likely.
She also knew at this point that the CDC was employing diagnostic techniques unable to identify viruses that had never before infected U.S. populations—they didn’t have the right testing materials. For a virus to show up on the panel of tests the CDC was using, it had to be a familiar one—like St. Louis virus.
McNamara pressed on, searching for organizations that had the resources to perform the right tests and that might be open to some form of collaboration. When a member of her team at the Bronx Zoo was exposed to the virus through an accidental encounter with a contaminated needle, McNamara’s campaign to enlist the help of any group with the diagnostic tools needed to identify the virus shifted into high-gear.
She left frequent updates for officials at the CDC in Fort Collins, Colorado.
No callbacks.
She sent tissue samples from the birds she necropsied to USDA’s National Veterinary Services Laboratory in Ames, Iowa—which did start testing, albeit with limited enthusiasm and resources—and to other independent labs.
On one occasion, over a weekend, McNamara even called the Plum Island Animal Disease Center, a former offshore army fort the government has used as an animal disease testing ground since 1956.
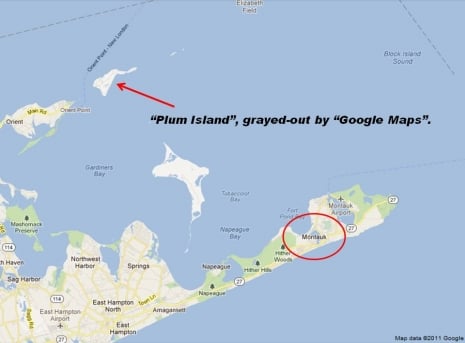 Instead of the rapid response movie-goers are trained to expect from officials manning this kind of exotic, frontline defense against foreign plague and pestilence, McNamara got a voice-mail message giving the caller a special ‘code’ to use in case of an emergency. McNamara dialed back five times—incredulous, she thought she might be dialing a wrong number—only to be informed, via recording, that the ‘code’ she’d keyed in was not working.
Instead of the rapid response movie-goers are trained to expect from officials manning this kind of exotic, frontline defense against foreign plague and pestilence, McNamara got a voice-mail message giving the caller a special ‘code’ to use in case of an emergency. McNamara dialed back five times—incredulous, she thought she might be dialing a wrong number—only to be informed, via recording, that the ‘code’ she’d keyed in was not working.
That weekend, at least, Plum Island was closed for business.
On September 21, 1999—roughly a month after the virus (or viruses, according to the CDC) surfaced in New York—McNamara decided to rattle the chain of command, and to reach out to personal contacts at the US Army Medical Research Institute for Infectious Diseases (USAMRIID) in Ft. Detrick, Md.
Unlike the CDC, USAMRIID, with its international reach, did possess the sophisticated testing capabilities McNamara needed to identify the strain of encephalitis killing crows and other birds at the zoo and to determine the relationship of that strain to what the CDC kept insisting had to be a ‘separate’ virus targeting human victims in New York.
USAMRIID
McNamara’s contacts at USAMRIID told her to rush tissue samples from the birds at the zoo to Ft. Detrick.
They also provided the pathologist and her team with the safety equipment (a BL-4 unit created for treating patients with the Ebola virus) McNamara’s team needed —a feat that still meant the zoo pathologist had to obtain supporting letters of request from federal agencies like USDA, since government agencies are not permitted, even during a dangerous outbreak of an unknown virus, to share equipment with private outfits like the Bronx Zoo.
In less than 24 hours, on September 22, USAMRIID ruled out Eastern Equine encephalitis, the virus the CDC told McNamara must be killing the birds.
Army researchers turned next to the St. Louis virus (SLE).
Although reagents to test the avian tissue demonstrated a weak correlation with SLE, viral experts at USAMRIID also knew that the virus that hit St. Louis in 1933 shared important characteristics with another strain—the West Nile virus, unknown, up to that point, in the US.
Also on September 22, researchers at USAMRIID determined that the sequences of genome fragments belonging to the West Nile virus and isolated from dead birds and mosquitoes were identical to gene sequences from the human autopsy specimens taken from the bodies of New Yorkers the CDC had said were killed by the St. Louis virus (SLE).
Here was the answer Tracey McNamara had been waiting for, confirmation that the dead birds from the Bronx Zoo had been infected, like their human counterparts in New York, by the same strain of virus—in this case, the West Nile virus, a rare form of encephalitis native to Africa and never before seen in the western hemisphere.
West Nile virus, let’s repeat, is transmitted not only by Culex pipiens, the same mosquitoes that carry St. Louis fever (SLE), but also by Anopheles mosquitoes and the Aedes vexans mosquito, which unlike the first two, is active during the day as well as night.
Third time around: Most of the pesticide spraying that had occurred in New York had been conducted in the evening, a fact that, remarkably, managed to escape the notice of the press and public.
Convergence
On the same day USAMRIID identified the West Nile virus, September 22, army researchers contacted officials in New York who had been working with the CDC and offered to share the results of their testing.
USAMRIID also offered to work with health officials in New York, but the reception was chilly: CDC told NYC health officials further input from Ft. Detrick was unnecessary. A better word might have been ‘unwelcome.’
Stovepiping again. Competition versus cooperation. During the same three weeks that Tracey McNamara spent contacting animal health organizations and working with her own contacts at USAMRIID, New York state and city health officials had been collaborating only with organizations whose mandates, like their own, limited them to the study of human disease.
Here was the real danger, McNamara knew, to the nation’s health and the ability of health officials at every level to cope with larger disaster. It was this wall between the study of human disease and animal disease that might be delaying a correct diagnosis of the disease attacking senior citizens and the avian population in New York, institutional self-interest that put the living at risk and growing numbers of victims in the ground.
On September 20, 1999, two days before McNamara’s colleagues at USAMRIID would confirm the disease as West Nile virus, CDC officials back at Fort Collins, Colorado, were beginning to worry their earlier identification of St. Louis virus (SLE) might have been a misdiagnosis.
CDC officials in Colorado had spoken to McNamara on September 10, but they had ignored her request to test samples from avian tissue, and failed to return any of her subsequent calls.
Even so, on September 20, increasing pressure to retest samples taken from human victims finally pushed CDC officials in Colorado to do what McNamara had urged them to do ten days earlier. They took avian samples the Bronx Zoo pathologist had sent to them via the NVSL in Iowa, and began to analyze them.
Around the same time, public health officials in New York—frustrated because they believed they had not yet received conclusive, “official,” results from the CDC—begun working with their own man, Dr. Ian Lipkin, Director of the Emerging Diseases Laboratory at the University of California-Irvine.

Dr. Ian Lipkin identifies WNV for CDC
Dr. Lipkin was testing human samples officials in New York had sent to UC-Irvine. Lipkin’s team used a molecular diagnostic technique available only at UC-Irvine, and relayed the results—which, unlike the CDC’s, were indisputable—to public health officials in Albany on September 23.
Three weeks after the Chief Pathologist at the Bronx Zoo had contacted the CDC, alerting them to her suspicions, and one day after army researchers at Ft. Detrick had zeroed in, diagnostically, on West Nile virus, this newest set of players at UC-Irvine were led by their own analyzes of largely human tissue to exactly the same diagnosis.
September 23—Lipkin flashes his findings to health officials in New York and the CDC: the virus affecting birds, mosquitoes, and human victims In New York was the never-before-seen in the US West Nile strain, not the St. Louis virus, as CDC had announced three weeks earlier, or Eastern Equine encephalitis, the disease CDC officials told McNamara was responsible for avian deaths at the Bronx Zoo.
On September 24, the State of New York Department of Health grabbed the headlines, issuing a press release trumpeting a breakthrough on the part of the national health system—“CDC Identifies New Encephalitis Virus in New York State.”
The release claimed CDC researchers in Colorado had discovered that the strain of encephalitis taken from avian tissue obtained in New York was, in fact, the West Nile virus, a “variant” so similar to the St. Louis virus (SLE), stressed a NYC-DOH spokesperson, that it is often called “Old World St. Louis encephalitis.”
The press release issued by New York City’s Department of Health made no reference to the fact that the samples had come to the CDC from the Bronx Zoo via NVSL in Ames, Iowa, to the part that Tracey McNamara or USAMRIID had played in the investigation, or to the involvement of Dr. Ian Lipkin at UC-Irvine.
On September 27, three days later, officials in New York addressed at least one of those omissions, crediting a collaborative effort between Lipkin and the CDC with the discovery of the West Nile virus in human patients. The follow-up release also contained a low-key correction regarding the CDC’s original diagnosis of St. Louis virus (SLE).
Lipkin, pleased by the public recognition belatedly accorded his team at UC-Irvine, also revealed that the CDC, newly-attuned to its inadequate diagnostic technology, had taken the precaution of contracting with the Emerging Diseases Laboratory at UC-Irvine in case its services were needed again.
Biosecurity–where is Congress?
Despite the media headlines declaring 2012 a banner year for West Nile virus, little seems to have been learned from the initial response of US health officials to the arrival of the disease in 1999.
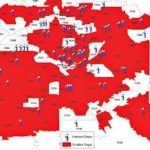
WNV map 2012
While USAMRIID, with its international resources, was pivotal in the identification of a new zoonotic pathogen, and critical to an understanding of the best responses to it, the legal wall we call posse comitatus prohibits the military from taking the lead on this or any other outbreak of disease that occurs ‘naturally.’
There is no organization, no budget, and no interest on the part of the Administration or Congress in establishing an agency focused on integrating human and veterinary medicine—providing active surveillance of wildlife vectors inevitably programmed to trigger human pandemics.
“If bioterrorists wanted to hit the US,” said McNamara shortly after army researchers nailed the West Nile virus, “this experience demonstrates the best way to do it would be to export a virus into this country by way of the ‘garbage population—mosquitoes, mice, rodents, etc.—and to initiate a disease that didn’t kill humans but destroyed animal populations important to the economy, pigs, cows, chickens, for example. Our experience with West Nile has proved the infrastructure we’d need to respond to that situation doesn’t exist in this country…the same thing could happen here that happened in the UK with mad cow disease.”
In 2012, McNamara is preaching a similar message, a warning about how the US government continues to prioritize and separate research into human disease from research into diseases affecting animals—and how those never-meeting twains may put our national security at risk.
McNamara recently proposed that $3 million be allotted for research into zoonotic disease, and the US government responded with a counter-offer of a few hundred thousand—a response impervious to the fact that more than half of the pathogens associated with emerging diseases, an urgent area of concern for biowarfare experts, are zoonotic—able to leap, in a single bound, from one species to another.
Not too long ago, Dr. Tracey McNamara told reporter Brendan Howard that “the system for discovering emerging zoonotic diseases has a long way to go. We have 18 state wildlife veterinarians and a few dozen federal veterinarians,” she said. “We need 90 to 100, and at least one state wildlife veterinarian per state. And we need the funding to support their work.” McNamara says the United States also needs better reporting across species for disease and better licensing for state and local wildlife staff who handle pathology work.
Finally—and this is fascinating—McNamara steps outside her usual comfort zone and admits there is at least one agency interested in strong animal and human health disease surveillance: the Department of Defense. The same sector that the CDC, the organization so reluctant to focus on emerging zoonotic disease, or to direct any significant part of its budget to wildlife pathology, no doubt sees as its primary competition.
Epidemiologists at Ft. Detrick no longer man the front lines in the fight against West Nile virus or the other zoonotic diseases against which the public seems to have little defense. They lay low, out of the limelight, in the rear. And so, at the end of the day, the question is whether a politicized bureaucracy like the CDC can abandon its own interests, and the interests of its executives, with the speed and focus it takes to combat an enemy as ruthless as the terrorists who took down the Twin Towers.
“West Nile virus-2012” should be required reading for the US Congress and the American people. Now. While 98 percent of the population of Dallas and surrounding cities is still alive and well.
Of course, there’s always next year.